You have tried everything. The visual schedule is on the wall. The timer is set. You used your calmest voice. You offered choices. And your child still will not brush their teeth. Not because they are being defiant. Not because you are doing something wrong. But because the very act of being asked to do something, anything, triggers a wave of panic they cannot control.
You have read the parenting books. You have sat through the therapy sessions. You have tried reward charts, first-then boards, countdowns, and every transition strategy recommended by well-meaning professionals. Some of them worked for a day. Maybe a week. Then your child figured out the system and the whole thing fell apart. Again.
If this sounds like your life, you are not failing. You may be parenting a child with a demand avoidance profile, sometimes called PDA, and it changes everything about how support needs to look.
What Is PDA and Where Did It Come From
PDA stands for Pathological Demand Avoidance, a term first used in 1983 by Professor Elizabeth Newson, a developmental psychologist at the University of Nottingham. She noticed a group of children who came in for autism assessments but did not quite fit the expected patterns. They were socially aware. They could make eye contact. They were imaginative. But they shared one overwhelming characteristic: an intense, pervasive need to avoid everyday demands.
Newson described these children as having "an obsessional avoidance of the ordinary demands of everyday life" and an overwhelming drive to maintain a sense of control. In 2003, she published her findings in the journal Archives of Disease in Childhood, based on a cohort of 150 children seen over 25 years, arguing that PDA should be recognized as a distinct profile within the autism spectrum.
Today, many families and clinicians use the term PDA profile to describe a pattern of demand avoidance that goes far beyond what you see with typical childhood resistance. Some autistic self-advocates have proposed the alternative name "Pervasive Drive for Autonomy," reframing the same behaviors through a lens of neurodivergent identity rather than pathology.
It is worth noting that PDA is not currently listed as a formal diagnosis in the DSM-5 or ICD-11. In the United Kingdom, where the concept originated, some clinicians diagnose "Autism Spectrum Disorder with a PDA profile." In the United States, awareness is growing through parent advocacy and social media, but formal clinical recognition has been slower to follow. A 2024 scoping review published in Frontiers in Education found only 22 studies on PDA across all research, with 21 originating from the UK. The research base is small, but for families living this every day, the description fits in a way nothing else has.
How Demand Avoidance Is Different from Defiance
This is the part that changes everything once you understand it. A child who is being defiant is making a conscious choice to resist authority. They know what is expected. They can do it. They are choosing not to, often out of anger, frustration, or a desire to test limits.
A child with a PDA profile is not choosing anything. Their nervous system is responding to a perceived threat. Every demand, no matter how small or how kindly delivered, activates the same fight-or-flight response you would feel if someone told you to jump off a cliff. The demand itself becomes the threat. Not the content of the demand. Not the person making it. The fact that someone expects something of them.
This is why PDA looks so different from what most parents and professionals expect. Your child might be fine playing independently, and then the moment you say "time to eat," a meal they actually want, they spiral. They might beg for a trip to the park and then refuse to put on shoes the instant the outing becomes a plan. They might desperately want to do their homework and sit frozen in front of it, unable to start, because now it is an expectation rather than a choice.
Dr. Cynthia Martin, a clinical psychologist at the Child Mind Institute, explains it this way: "Any external demand that is coming from somebody else, or that the person perceives is coming from another person, that generates a lot of internal discomfort, which leads to the avoidance."
This is fundamentally different from Oppositional Defiant Disorder, or ODD, which is sometimes confused with PDA. ODD involves deliberate resistance, often directed at specific people or authority figures, rooted in anger or frustration. PDA is anxiety-driven and pervasive across all settings, all people, and all types of demands, including ones the child places on themselves. Perhaps the most important clinical distinction: the strategies that work for ODD, structured consequences, firm boundaries, reward-and-punishment systems, actively make PDA worse.
The Signs That Traditional Strategies Are Not Working
If your child has a PDA profile, you have probably noticed a pattern. Things that "should" work, based on everything you have read about autism supports and behavioral strategies, either fail or backfire.
Reward charts lose their power fast. Sticker charts, token systems, and point-based rewards might generate initial enthusiasm. But within days or weeks, the system itself becomes a demand. Earning stars means complying, and compliance is the thing their nervous system is fighting against. Dr. Martin notes: "When we are only taking a heavy behavioral approach, where it is very reward-and-consequence driven, we often see treatment effects that are high initially, but then taper off over time."
Firm boundaries trigger escalation, not compliance. Where a neurotypical child might push back and then comply when they see you are serious, a PDA child reads escalation as a bigger threat and responds with bigger avoidance. What started as ignoring becomes arguing, then crying, then a full meltdown. They are not testing you. They are panicking.
Predictable routines become predictable demands. One of the most confusing parts of PDA for parents of autistic children is that routine and structure, normally a cornerstone of autism support, can become the enemy. Once a visual schedule becomes "the thing I have to do every morning," it stops being helpful and starts being another source of anxiety.
Praise feels like pressure. You would think a child would welcome recognition for doing something well. But for a PDA child, "Great job brushing your teeth!" can register as an expectation to do it again tomorrow. Even positive attention can feel like a demand for repeat performance.
They avoid things they genuinely want to do. This is the hallmark that confuses everyone. Your child asks to go swimming. You start getting ready. They refuse to put on a swimsuit. They are not being difficult. The thing they wanted became a series of demands the moment it became a plan, and their nervous system shut it down.
What Demands Actually Look Like Through a PDA Lens
Most people think of demands as instructions. "Clean your room." "Do your homework." "Eat your vegetables." But for a child with a PDA profile, the category of "demand" is far broader than anyone expects.
Direct demands are the obvious ones. "Brush your teeth." "Put on your shoes." "Come to the table." These are the requests most parents try to soften first, and they are often the easiest to work around with alternative strategies.
Indirect demands are trickier. Questions can feel like demands because they require a response. "What do you want for lunch?" forces a decision. Compliments can feel like demands because they set expectations. Transitions of any kind create demands because they require shifting from what is happening now to what needs to happen next. Even time itself is a demand. Knowing that something is scheduled for 3:00 PM means having to be ready at 3:00 PM, and that alone can trigger avoidance hours in advance.
Internal demands are the ones that catch families off guard the most. Hunger is a demand because it requires action. Needing the bathroom is a demand. Feeling tired is a demand. A child may genuinely want to eat their favorite food and find themselves unable to do it because the wanting has turned into a need, and the need has become a demand they cannot meet. This is not stubbornness. It is a nervous system that treats even self-generated expectations as threats.
What Actually Helps: Strategies That Work With PDA
The PDA Society in the UK developed a framework called PANDA that captures the core principles of effective support for demand-avoidant children. It stands for Pick battles, Anxiety management, Negotiate and collaborate, Disguise demands, and Adapt flexibly. These are not techniques you apply rigidly. They are a way of thinking about your child that shifts the entire dynamic.
Pick Your Battles Ruthlessly
Every rule you enforce adds to your child's internal demand load. Ask yourself: does this actually matter right now? If the answer is no, let it go. Your child wearing mismatched socks to school is not worth the meltdown that comes from insisting they change. Eating cereal for dinner is not a nutritional crisis. Doing homework on the floor instead of at a desk is fine.
This is not permissive parenting. It is strategic parenting. You are preserving your child's capacity for the demands that genuinely matter, like safety, hygiene, and getting to school, by removing the weight of demands that do not.
Lower Anxiety as the First Priority
If your child is already dysregulated, no strategy will work. The first job is always to bring the emotional temperature down. Speak slowly. Use a calm, even tone. Keep your body language soft and open. Do not stand over them. Get on their level. Give them space if they need it. Wait. The demand can come later, after the nervous system has calmed.
A 2021 meta-analysis found that 46% of caregivers of autistic children show significant stress levels, with 44.6% reporting anxiety. When your own nervous system is activated, your child's activation increases. Managing your own regulation is not a luxury. It is part of the strategy.
Use Declarative Language Instead of Commands
This is one of the most powerful shifts you can make. Declarative language shares information or makes observations rather than giving instructions. It invites the child to respond rather than demanding they comply.
Instead of "Put your shoes on," try "I notice it is chilly outside today." Instead of "Brush your teeth," try "The toothbrush is on the counter." Instead of "Time to leave for school," try "I wonder what we need before heading out." Instead of "Come eat dinner," try "Dinner is on the table."
You are still communicating the same information. But you are removing the demand wrapper. The child gets to process the information and choose to respond rather than feeling forced into compliance. This does not work every time. Nothing works every time with PDA. But it works more often than direct commands.
Enjoying this article?
Get practical tips and insights delivered to your inbox — no spam, ever.
Disguise and Depersonalize Demands
When a demand does need to happen, make it feel like it is coming from somewhere other than you. Use timers, visual cues, or external rationales. "The schedule says it is time for bath" feels different from "I need you to take a bath." The schedule is the authority, not you. That small shift in perceived source can make the difference between cooperation and collapse.
Humor works surprisingly well. "I bet you cannot get your pajamas on before I count to twenty" turns a demand into a challenge. Roleplay works too. "Your teddy bear needs to show you how to brush teeth tonight" puts the demand on a character instead of the child.
VizyPlan can serve as that external reference point. When the app shows the next step in a routine rather than a parent giving a verbal instruction, the demand feels less personal. The key is that the child participates in building the routine so it feels collaborative rather than imposed.
Collaborate, Do Not Dictate
Dr. Ross Greene, developer of the Collaborative and Proactive Solutions model, built his entire approach around one principle: "Kids do well if they can." When children are not meeting expectations, it is because they lack the skills or capacity to do so in that moment, not because they lack motivation.
His approach has three steps. First, empathize: listen to your child's concerns about the situation without judgment. Second, define the problem: share your concern calmly and clearly. Third, invite collaboration: work together on a solution that addresses both concerns. This works well for PDA because it directly honors the child's core need for autonomy and control. You are not imposing a solution. You are building one together.
Adapt Constantly
Here is the part that exhausts parents: what works today may not work tomorrow. A strategy that successfully got your child through morning routines for two weeks can suddenly become a demand itself once it becomes an expectation. You may need to rotate approaches, change the order of routines, use different language, or take a completely different route to the same outcome.
This is not a failure of the strategy. It is a feature of PDA. Flexibility is not optional. It is the strategy.
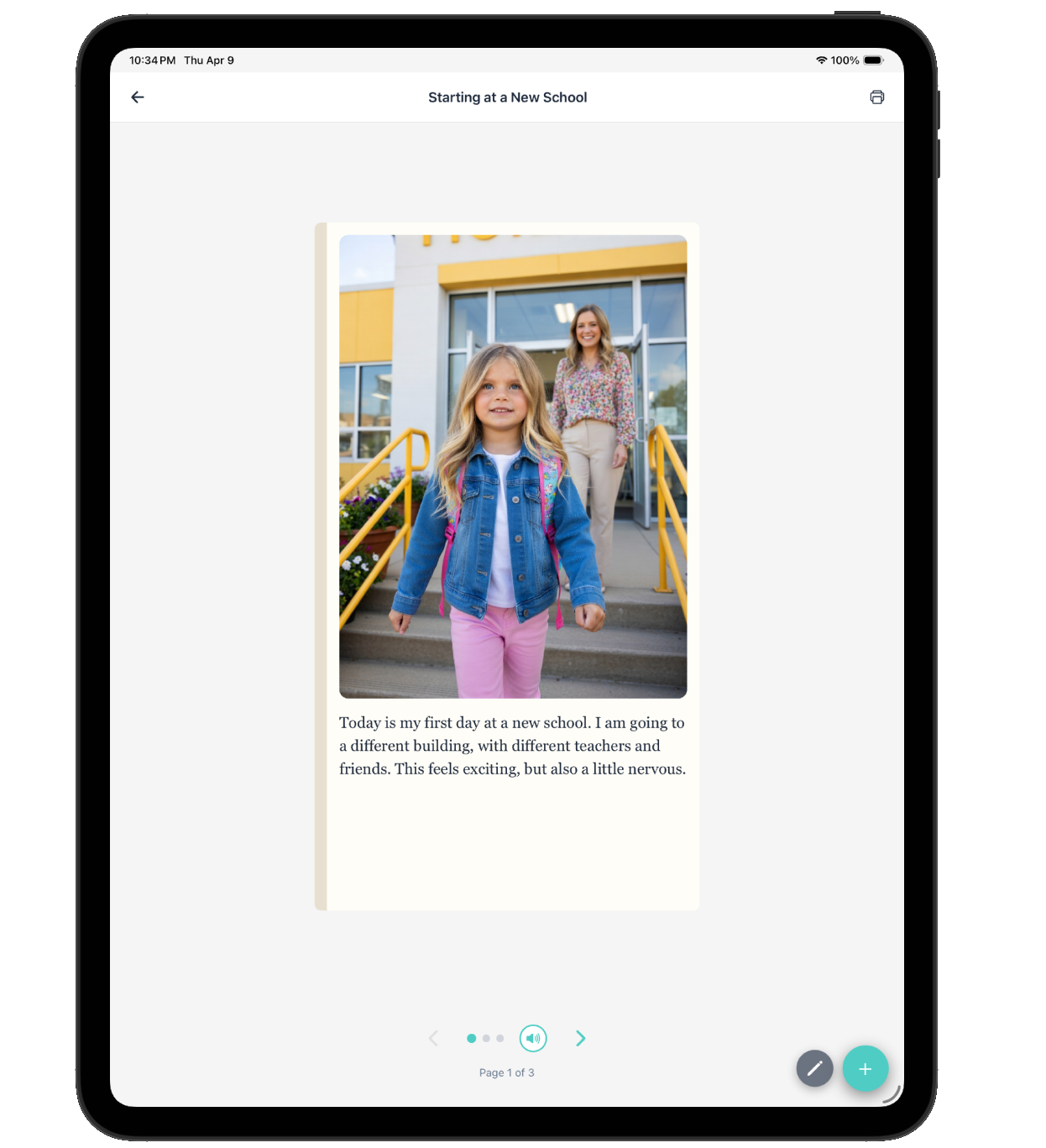
Rethinking Visual Supports for Demand Avoidant Children
If you have tried visual schedules and they did not work, it may not be that visual supports are wrong for your child. It may be that the visual supports were presented as a fixed list of demands rather than a flexible framework.
Traditional visual schedules tell a child "here is what you are doing, in this order, and you need to do all of it." For most autistic children, that predictability is calming. For a PDA child, it is a wall of demands staring them in the face.
Adapted visual supports for PDA look different. They show options rather than requirements. They invite the child to participate in planning. They use "here is what is happening today" language rather than "here is what you need to do." They include choice points where the child selects what comes next. They can be rearranged, modified, or simplified on the fly.
VizyPlan works well for this approach because routines can be customized, reordered, and updated quickly. When your child helps build their own visual routine using personalized AI-generated images of themselves doing each step, the routine feels like theirs rather than something imposed on them. That sense of ownership can be the difference between avoidance and engagement.
The Misconceptions That Hurt Families Most
Parents of PDA children face a unique form of isolation. The behavior looks like defiance to outsiders, which means the advice you get from family, friends, and sometimes even professionals centers on being firmer, more consistent, more authoritative. Exactly the approach that makes things worse.
"They are manipulating you." PDA behaviors can look strategic. Your child may use distraction, negotiation, excuses, even charm to avoid demands. But these are not manipulation tactics. They are survival strategies. A child drowning does not "manipulate" the water. They do whatever they can to stay afloat. Your child is doing the same with their nervous system.
"You just need firmer boundaries." This advice comes from people who have never watched a child unravel because they were asked to put on socks. More pressure does not create more compliance with PDA. It creates more panic, bigger meltdowns, and deeper withdrawal.
"They will grow out of it." A 2016 study using the DISCO diagnostic interview found that 44% of individuals with PDA features showed improvement over time. That is encouraging, but it also means more than half carry these traits into adolescence and adulthood. PDA is not a phase.
"It is bad parenting." Research consistently shows that demand avoidance is neurologically based. You did not cause this. The fact that you are reading an article like this, trying to understand your child better, is evidence of exactly the opposite.
When PDA and Other Profiles Overlap
Demand avoidance does not exist in isolation. Many children with PDA profiles also have co-occurring ADHD, anxiety, or sensory processing differences that compound the challenges.
A child with PDA and ADHD may have even more difficulty with transitions because both their demand sensitivity and their executive function challenges are working against them. A child with PDA and sensory sensitivities may avoid getting dressed not only because getting dressed is a demand but because the clothing itself is intolerable.
Understanding which challenges are demand-related and which stem from other aspects of your child's neurodivergent profile helps you target the right strategies. The demand avoidance piece needs low-demand, autonomy-supporting approaches. The sensory piece needs sensory accommodations. The executive function piece needs scaffolding and visual supports. Most PDA children need all of these working together.
Finding Professional Support That Understands PDA
Not every therapist or clinician will be familiar with PDA. In the United States especially, the concept is still gaining recognition. When looking for support, ask potential providers directly: "Are you familiar with the PDA profile? How does it change your approach?"
A provider who understands PDA will talk about flexibility, collaboration, and autonomy rather than compliance and consequences. They will not suggest that you "just need to be more consistent" or recommend a rigid behavioral program. They will recognize that traditional approaches need significant adaptation for demand-avoidant children.
If your child has been diagnosed with ODD and the recommended treatment is not working, consider seeking an evaluation specifically for autism with a PDA profile. The strategies that help these two presentations are fundamentally different, and using the wrong approach can do more harm than doing nothing at all.
What This Means for Your Family Right Now
Understanding PDA does not make the daily struggles disappear. Your mornings will still be hard. Transitions will still be challenging. There will still be days when you cannot get your child to do the thing they desperately need to do.
But understanding what is driving the behavior changes how you respond to it. Instead of thinking "my child is fighting me," you start thinking "my child's nervous system is in threat mode." Instead of adding more structure, you look for ways to reduce perceived demands. Instead of feeling like a failure when strategies stop working, you adapt and try something different, knowing that flexibility is the strategy.
One mother in a 2025 study published in Discover Mental Health described the moment she learned about PDA: everything suddenly made sense. Years of confusion, guilt, and strategies that should have worked but did not finally had an explanation. That moment of understanding does not fix the practical challenges. But it changes the emotional landscape of parenting entirely.
Your child is not broken. They are not defiant. They are not choosing to make your life difficult. They have a nervous system that perceives demands as threats, and they need you to be the person who understands that when no one else does.
You are already that person. You are here. You are learning. And that matters more than any strategy in any book.
VizyPlan helps you create flexible visual routines, track patterns that reveal your child's triggers, and build supports that feel collaborative rather than controlling. Start your free trial and discover what happens when visual supports are built with your child, not just for them.